
We make compliance straightforward with nationwide, HSE-compliant asbestos medicals delivered by fully accredited doctors and backed by the UK’s largest fleet of mobile health units. Whether you need one assessment or a full workforce programme, we’re here to help you stay ahead of risk and regulation.
Trusted by over 3,800 businesses









Who Needs an Asbestos Medical?
Anyone who works with or is exposed to asbestos fibres during the course of their job is legally required to undergo regular asbestos medicals. This applies to both licensed and non-licensed asbestos work. The first medical must be completed before starting work with asbestos, and then every two years thereafter, or sooner if there are any health concerns.
What’s Included in an Asbestos Medical?
- Conducted by HSE Appointed Doctors
- Detailed occupational health assessment
- Chest examination
- Lung function testing
An Asbestos Medical is a form of Health Surveillance legally required for employees who carry out licensable asbestos work in the UK, and in some cases, for Notifiable Non-Licensed Work (NNLW). The purpose is to monitor employees for early signs of potential health problems caused by their work and to ensure they remain fit to work with asbestos safely.
The examination is conducted by a doctor appointed by the Health and Safety Executive (HSE).
Key Components:
- Medical and Occupational History Review: Detailed discussion of past and present work, especially concerning asbestos exposure (level, frequency, and duration).
- Respiratory Health Review: Assessment of current symptoms related to breathing, coughing, and chest pain.
- Physical Examination: A focus on the respiratory and cardiovascular systems, particularly the chest examination.
- Lung Function Testing: Use of a spirometer to measure lung performance.
- Further Tests (If Indicated): The appointed doctor may recommend a Chest X-ray or other imaging if specific abnormalities or concerns are noted.
- Certification and Advice: Provision of an HSE-approved medical certificate and advice on fitness to work, continued exposure, and the importance of using Respiratory Protective Equipment (RPE) correctly.
The initial part of the medical is a comprehensive assessment designed to establish an individual’s exposure history and current health status.
Medical History: The doctor reviews your full medical history, noting any pre-existing conditions (e.g., asthma, COPD, smoking status) that could affect your lungs or cardiovascular system, as these can impact fitness to wear RPE or complicate the assessment of asbestos-related disease.
Occupational Exposure History: This is critical. The doctor needs to know:
- When and where the exposure occurred.
- Type of work performed (e.g., licensed removal, surveying, maintenance).
- Duration and intensity of exposure.
- What control measures and RPE were used.

Respiratory Health Review: This involves discussing any new or worsening respiratory symptoms, such as:
- Shortness of breath (dyspnoea), especially on exertion.
- Persistent cough.
- Chest pain or tightness.
- Wheezing.
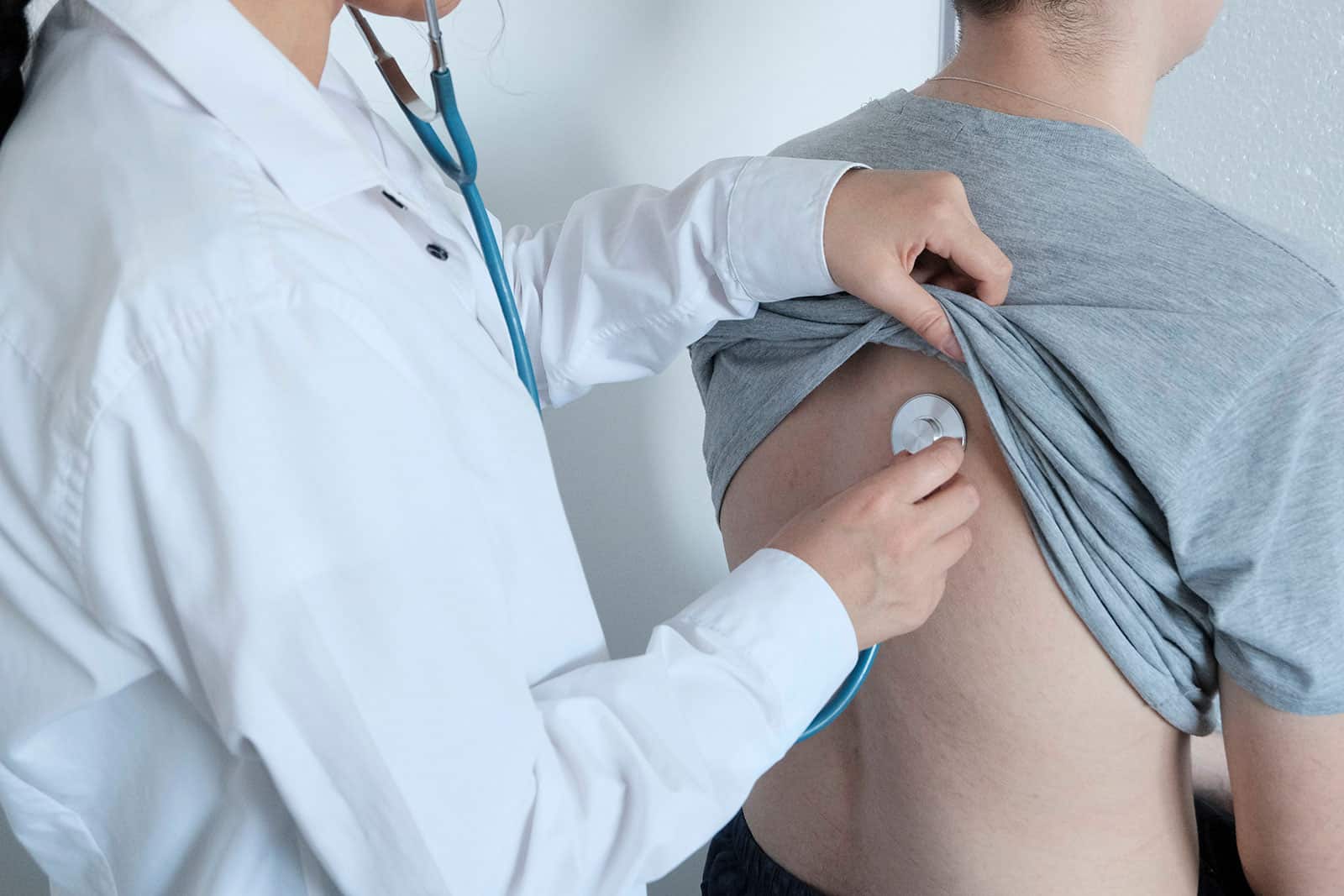
The physical chest examination is a fundamental part of the medical to look for early clinical signs of asbestos-related lung disease.
The doctor will perform auscultation, which means listening carefully to the sounds of your lungs using a stethoscope.
- Detection of Crackles: The primary focus is listening for a specific sound called “bibasal crackles” or crepitations. These are dry, crackling noises heard during inhalation, usually at the base of the lungs. The presence of crackles can be an early sign of Asbestosis (scarring of the lung tissue).
- General Chest Assessment: The doctor will also assess your overall chest shape, movement during breathing, and may check for signs like finger clubbing, which can be associated with chronic respiratory disease.

Spirometry is a non-invasive, objective test that measures how well your lungs are working. It’s a standard tool in health surveillance for workers exposed to respiratory hazards, including asbestos.
What Spirometry Measures:
The test measures two key volumes, which help identify common patterns of lung impairment:
- Forced Vital Capacity (FVC): The total amount of air you can forcefully exhale after taking the deepest possible breath. A reduction in FVC can indicate a restrictive defect (like asbestosis), where the lungs are stiff and unable to fully expand.
- Forced Expiratory Volume in 1 Second (FEV1): The amount of air you can forcefully exhale in the first second. A low FEV1 often points to an obstructive defect (like asthma or COPD), where the airways are narrowed.
- FEV1 / FVC Ratio: The ratio of the two measurements, which is key in differentiating between obstructive and restrictive defects.
How the Test is Performed:
The employee sits comfortably and is asked to:
- Take the deepest possible breath in.
- Blow as hard and fast as they can into a mouthpiece connected to the spirometer machine, until their lungs are empty.
- The test is usually performed multiple times (e.g., three acceptable attempts) to ensure the results are reliable and accurate.
Importance for Asbestos Workers:
Regular spirometry (typically every two years for licensed work) allows the occupational health professional to track changes in lung function over time. Catching a decline in FVC, FEV1 or the ratio early is vital, as it allows for prompt intervention, advice, and a review of workplace controls to prevent further health deterioration.

Let’s Get You Started
Our occupational health specialists will guide you from first contact to full deployment without the jargon, delays, or disruption. Complete our quick form and our team will be in touch.



